Brain tumour treatment
When your doctor gives you a diagnosis, they will often tell you what the next step will be in terms of brain tumour treatment. In many cases treatment might even begin on the same day as a diagnosis, leaving you little or no time to prepare for what you will go through. The information we provide is aimed at preparing you for every stage of brain tumour treatment, whether it’s for you or someone you care for.
Conventional brain tumour treatments
Brain tumour treatment can include surgery, radiotherapy, chemotherapy, steroids, and more. But, the type of treatment will depend on a number of factors such as the type of tumour, its location, and the person affected by the brain tumour.
Brain tumour treatments for adults and children can differ slightly. And, there are complementary treatments to consider. Below we have some information on child and adults brain tumour treatment types, along with some of the therapies that could accompany them.
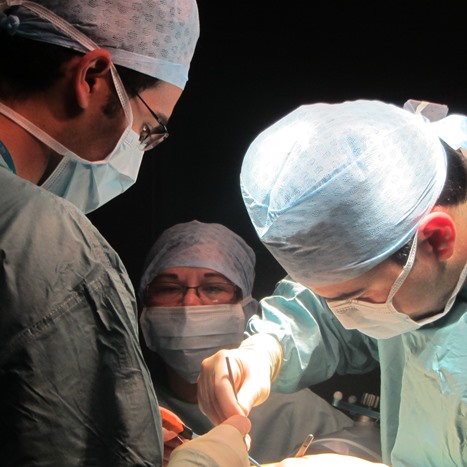
Child treatments
Information about different brain tumour treatments available for children.

Adult treatments
Information about different brain tumour treatments available for adults.

Complementary treatments
Therapies used alongside conventional treatments to help manage side-effects.
Non-conventional brain tumour treatments
When you, or someone you love, is diagnosed with a brain tumour, you might find yourself searching for new or experimental brain tumour treatments. Looking for anything that could help is completely understandable.
But, it’s important to be aware of the information you’re finding, and where it comes from. Some information comes from trusted sites and is evidence-based and fact checked by experts in the field. But, a lot of the information out there is just people’s opinions or anecdotes and doesn’t have any evidence to back it up.
While it’s tempting to want to believe anything that seems to apply to you or your loved one, sometimes the information can be misleading and can actually cause harm.
So, if you find anything that you think could help your brain tumour treatment, it’s best to discuss it with your healthcare team before trying it. They may be able to give you further information and advise if it will interact and impact any of your current treatment or medications.

Emerging treatments
Read about some of the new brain tumour treatments currently in development.

Accessing unlicensed drugs for brain tumours
Some patients might be able to access promising unlicensed drugs outside clinical trials to treat brain tumours.

Vitamins and supplements
Some people believe certain vitamins, supplements or diets might help improve their outcome

Get your free Information Pack today
If you or someone you love has been diagnosed with a brain tumour and you don’t know which way to turn, start with our Information Pack.