High grade tumour research update
For people and families affected by the diagnosis of a high grade brain tumour, we know that a cure really can’t wait. That’s why we invest in cutting-edge research to make discoveries, propel them into the clinic and drive new treatments.

Our researchers are finding the origins of Medulloblastoma, testing new drugs for DIPG, discovering new ways to stop GBM growth and developing tools for predicting aggressive Meningioma recurrence. We want to share their progress with you here.
We’re excited to share the latest progress from a selection of those grants below. At the end of each progress update you’ll find the link to the grant’s own webpage where there’s more information.
Targeting ALK2 inhibitors for DMG (formerly known as DIPG)
Lead researcher: Dr Alex Bullock
Where: Structural Genomics Consortium, Oxford
Cost: £491,051 over four years
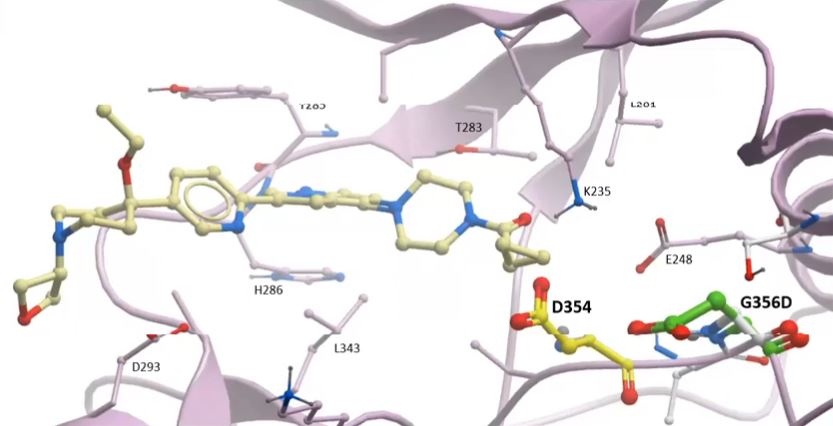
To date, the research has produced about 400 chemicals that have potential as DMG drugs. In Oxford, researchers have tested these the lab to assess:
- how tightly they bind to the intended target, the ALK2 protein;
- whether they do this specifically (desirable) or bind equally to other proteins which may cause toxicity; and
- how well they kill DIPG cells.
Progress is shared regularly at monthly team meetings which are recorded and shared on YouTube as well as through a blog with a lab notebook.
Click to view the latest progress video.
Most encouragingly, Dr Bullock’s team have identified a group of potential drugs that bind strongly to ALK2 and cause patient-derived DMG cells to grow more slowly. From these, the researchers will focus on five top drug candidates that will be further investigated with the ultimate aim of getting them into clinical trials.
Since this project started the research has been going so well that the researchers have set up a new company, called Meds4Kids, to drive the potential drugs through the next stage of development and on to clinical trials.
Origins of medulloblastoma
Lead researcher: Dr Laure Bihannic
Where: St Jude Children’s Research Hospital, Memphis USA
Cost: £180,000 over three years, initially
Dr Laure Bihannic started this three-year grant in September 2018. This grant was awarded as part of our Future Leaders funding, which has the overall aim of growing the field of researchers working on brain tumours and ultimately bringing them to the UK. In line with this she will be eligible to apply for further funding at the end of her current grant.
Cell of origin
Dr Bihannic has studied cerebellar development using a new technology known as single-cell RNA sequencing. This approach identified individual cerebellar cell types present during the development of the murine cerebellum. She then studied patient MB using the same technique (i.e. single-cell RNA sequencing).
By comparing the tumour cells and the developing cerebellar cells she identified two cell populations as highly similar to Group 4 medulloblastoma. These cell types are glutamatergic cerebellar nuclei (GluCN) and unipolar brush cells (UBCs), suggesting that they might be the cells from which Group 4 tumours originate. They will now isolate these cells in their models to study them in more depth.
Functional validation of medulloblastoma subgroup origins
The goal of the work above is to determine the normal cerebellar cell populations most similar to human tumour counterparts. These efforts, although necessary, will be insufficient to definitively prove cellular origin without direct functional evidence. After proposing the subtype-specific cell of origin, Dr Bihannic will endeavour to grow them in the lab in a way that mimics the childhood disease.
Her future studies will disturb the Group 4 medulloblastoma candidate populations, GluCN and UBCs, by overexpressing genes that have been implicated in Group 4 medulloblastoma formation. The ultimate aim would be to prove these cells cause tumours by implanting them in pre-clinical models and monitoring them for signs of tumour initiation.
Proteins as drug targets for glioblastoma
Lead researcher: Professor Steve Pollard
Where: University of Edinburgh
Cost: £1.48 million over 5 years
Chromatin regulators control gene expression. These proteins regulate the entire process of DNA being wrapped tightly into chromosomes. Chromatin regulators carry the important genetic information that controls how the cells in our body behave. If these regulators become mutated, it changes the way the DNA is wrapped, causing the cell to behave differently.
Professor Pollard’s team are paying particular attention to Trithorax group proteins (a chromatin regulator), aiming to identify which of the 1,000 chromatin regulators should be prioritised for drug development.
To study these proteins they’re testing drugs that have already been approved for use in other human diseases to see if they can target the chromatin regulators. These drugs have already been approved for use in humans, so if proven they’ll reach brain tumour patients much faster.
The research team are approaching this from two different directions.
- Firstly, using a candidate approach, harnessing existing knowledge of the most likely targets for drug development.
Existing small molecules (chemicals that could be used as drugs) are identified as candidates and are tested directly on normal and tumour cells.
- Secondly, exploiting the latest ‘genome editing’ technologies.
Genome editing enables the team to screen a large number of genes, and in parallel to identify those that would be priority for drug development.
In this second year of the project Professor Pollard and his team have optimised the methods needed to tackle the ambitious goals of this project. They have performed successful chemical and genetic screens, which have uncovered a wealth of potential new targets to follow up, including uncovering new gene switch regulators.
We have shifted attention to a specific target that might be expressed only in the brain stem cells – this would make it a better therapeutic target with less risks of toxicities in other tissues and organs.
Professor Steve Pollard
Encouragingly, the chemical screening has shown that a family of molecules known as HDACs are important to maintaining the key features of GBM stem cells that underpin their growth. The next avenue of research for this investigation is to inhibit HDACs, in combination with other drugs, and determine if that slows or stops GBM models growing in the lab.
Targeting clinically challenging meningiomas
Lead researcher: Dr Gelareh Zadeh
Where: University Health Network, Toronto, Canada
Cost: £1.5 million over five years
This research aims to improve our understanding of aggressive meningiomas and provide a foundation for more accurate diagnoses and treatments. The collaborative research programme is assembling experts in pathology, neurosurgery, genetics, and molecular biology from Canada, the UK, and USA. In addition, this programme will enable researchers to establish an international meningioma consortium with 14 collaborating institutes.
Dr Zadeh’s team have now completed genetic and epigenetic sequencing of over 150 meningioma tumour samples making this the most richly annotated cohort of samples that exists to date.
Excitingly, this work has enabled the creation of a clinical tool that helps predict the risk of tumour re-growth, for individual patients, after surgical removal.
Patients are now able to find out their own personalized risk of tumor growing back within 5-years once their tumour is removed by surgery. This represents a major advance in prognostication for meningiomas, and will impact whether or not patients would consider receiving radiation therapy after surgery to reduce the risk of tumor regrowth.
Dr Gelareh Zadeh
The work that led to the recurrence prediction tool has now published in the journal Neuro-Oncology and has been presented at several international neurosurgical and neuro-oncology conferences. The researchers have also filed a provisional patent for the recurrence prediction tool.