Oligodendroglioma
Oligodendrogliomas account for roughly 3% of all primary brain tumours. They are more common in adults, particularly those aged 40-60. They are usually grade 2 or grade 3. Because of this, there are various treatment methods, which we discuss here.
Short summary
Oligodendroglioma is a type of brain tumour that develops from the brain’s glial cells. It is a primary brain tumour, which means it starts in the brain as opposed to spreading there.
These tumours can be either low grade or high grade. Because of this, treatment can range from ‘watch and wait’ to neurosurgery, radiotherapy, and chemotherapy.
Oligodendroglioma symptoms usually depend on where the tumour is located in the brain, but could include the sensation of strange smells or muscular weakness.
On this page, we’ll discuss in detail:
- What is an oligodendroglioma?
- What are the symptoms of an oligodendroglioma?
- How is an oligodendroglioma treated?
- What causes oligodendroglioma?
- How long can I live with an oligodendroglioma?
Get support
If you have any questions or just need someone to talk to, please get in touch with our friendly and knowledgeable Support Team.
Get your free Information Pack
Our Brain Tumour Information Pack can help you better understand your diagnosis and feel confident talking to your medical team.
Get the BRIAN app
BRIAN is our trusted online app where you can track your experience, compare it with others who’ve been there and get the knowledge you need to make informed decisions.
What is an oligodendroglioma?
An oligodendroglioma is a primary brain tumour that is a type of glioma, meaning that develops from the glial cells in the brain. Oligodendrogliomas are primary brain tumours that are a type of glioma. They’re the third most-common glioma, accounting for around 3% of all primary brain tumours and 5-18% of gliomas.
The majority of oligodendrogliomas occur in the frontal lobe. The second most common site affected is the temporal lobe, followed by the parietal lobe.
They’re more common in adults, particularly in people aged 30-50, and are slightly more common in men than in women.
Oligodendrogliomas are diagnosed with 2 grades:
- grade 2 oligodendrogliomas, which grow slowly
- grade 3 oligodendrogliomas, which grow faster and are more likely to spread within the brain.
What are the symptoms of an oligodendroglioma?
Oligodendrogliomas may cause any of the symptoms common among brain tumours, particularly:
- seizures
- altered sensations, like strange smells or hallucinations relating to sense of smell
- muscular weakness, particularly down one side of the body, and loss of control of bodily movements.
Often, oligodendroglioma symptoms depend on where the brain tumour is located.
In the frontal lobe, oligodendrogliomas can cause gradual changes in mood and personality, and weakness or numbness in the muscles of one side of the body.
If it is located in the temporal lobe, this may cause problems with speech, coordination and memory.
How is an oligodendroglioma treated?
As grade 2 oligodendrogliomas grow slowly, you may be put on active monitoring (also known as watch and wait) if no treatment is required immediately.
If the tumour is large or causing symptoms that affect your quality of life, neurosurgery may be performed to remove as much as possible. This may be followed with radiotherapy or chemotherapy.
Grade 3 oligodendrogliomas are usually treated with surgery soon after diagnosis. This is usually followed by a combination of radiotherapy and chemotherapy because oligodendrogliomas are often ‘diffuse’, which means they’re more difficult to remove completely.
There are two genetic alterations that are almost always present in oligodendrogliomas: mutation in IDH1 or IDH2 genes, and co-deletion of chromosome arms 1p and 19q.
Detecting these genetic alterations with biomarker testing is now essential for diagnosis and when evaluating which treatments will be used for people who are diagnosed with an oligodendroglioma.
-
What is the 1p/19q test?
The test is useful in diagnosing oligodendrogliomas and, therefore, in making decisions about the most appropriate treatment for you.
How does the test work and what does it show?
Our bodies are made up of cells. Each cell has 23 pairs of chromosomes, which carry your genes (DNA). One chromosome of each pair is inherited from your mother, and the other from your father. Each pair of chromosomes are numbered 1 to 22, then XX or XY.
The 1p/19q test looks at genetic changes to chromosomes 1 and 19 to see whether they have a section missing. If the sections called the p section (p for “petite”, i.e. the shorter) of chromosome 1 and the q section (q has been chosen because it is the next letter in the alphabet) of chromosome 19 are missing, this means that the genes carried in those sections are also missing.
These genes seem to be involved in resistance to chemotherapy drugs. So if you’re found to be missing both those sections, you’re more likely to have a better response to chemotherapy and longer overall survival.
-
What is the IDH1/IDH2 test?
This test is useful in diagnosing oligodendrogliomas and in making decisions about the most appropriate treatment for you.
It might also be useful in predicting how effective a particular treatment is likely to be.
How does the test work and what does it show?
IDH1 and IDH2 are genes. A change (mutation) in the IDH1 or IDH2 genes has been found in almost all oligodendrogliomas and astrocytomas.
Tumours that have the change are known as IDH–mutant, and those without the change are known as IDH-wildtype.
Previously, a type of brain tumour called glioblastoma was divided into primary and secondary types. Secondary glioblastomas were those that had developed from a lower grade tumour and had an IDH mutation, whilst primary glioblastomas were those that developed without a lower grade tumour found beforehand, and were IDH-wildtype. It is now known that any adult-type diffuse gliomas (oligodendrogliomas, astrocytomas and glioblastomas) that have an IDH mutation tend to have better long-term survival.
So, in the most up to date tumour classification system, only oligodendrogliomas and astrocytomas will have IDH mutations and all glioblastomas are IDH-wildtype.
It’s important to be aware that people with gliomas that have the IDH1/IDH2 mutation tend to be younger adults and older children, which may partially account for their longer survival.
-
What is the MGMT methylation test?
For people with oligodendroglioma, the MGMT methylation test helps to predict how effective chemotherapy treatment is likely to be, although there are many other factors that also affect response to treatment. This can be used to help plan a suitable, individualised treatment plan.
What does the test show?
In summary, the test looks at the amount (percentage) of something called methylation. If your tumour is found to be:
- MGMT methylated, you’re more likely to respond well to TMZ chemotherapy.
- MGMT unmethylated, you’re less likely to respond to TMZ chemotherapy.
This helps your healthcare team decide on the best course of treatment for you. For example, if your tumour is unmethlyated, giving you high doses of chemotherapy may give you lots of unpleasant side-effects, but with little benefit in terms of reducing your tumour.
If you do decide to have the test, you need to be aware that it may be found to be unmethylated. Speak to your healthcare team about what would happen next if this turned out to be the case.
There are other factors that influence the effectiveness of chemotherapy, so there’ll always be ‘good’ and ‘poor’ responders in both the methylated and unmethylated groups.
-
TERT promoter mutation test
When found with 1p/19q co-deletion and IDH-mutant biomarkers, the TERT promoter mutation suggests a diagnosis of oligodendroglioma, and predicts greater benefit from chemotherapy and radiotherapy and longer survival, particularly in grade 2 and 3 gliomas.
However, when the TERT mutation is found on its own in grade 2 and 3 gliomas without mutations in the IDH1 or IDH2 gene, it usually predicts poorer survival. This suggests the need for early, more aggressive treatment.
What causes oligodendrogliomas?
As with most tumours, the exact cause of oligodendrogliomas is not known, although we do understand some of the risk factors.
This can be a difficult thing to accept and can leave you feeling helpless, but there is nothing you could have done to prevent this from happening.
The Brain Tumour Charity is contributing to the funding of research into the possible causes of brain tumour development as we accelerate towards a cure.
How long can I live with an oligodendroglioma?
Because they can be either grade 2 or grade 3, oligodendrogliomas don’t have a clear outcome. How you are affected depends on the details of your particular case.
However, we do have information on prognosis and survival rates. To find out more, you can click through to our oligodendroglioma prognosis page.
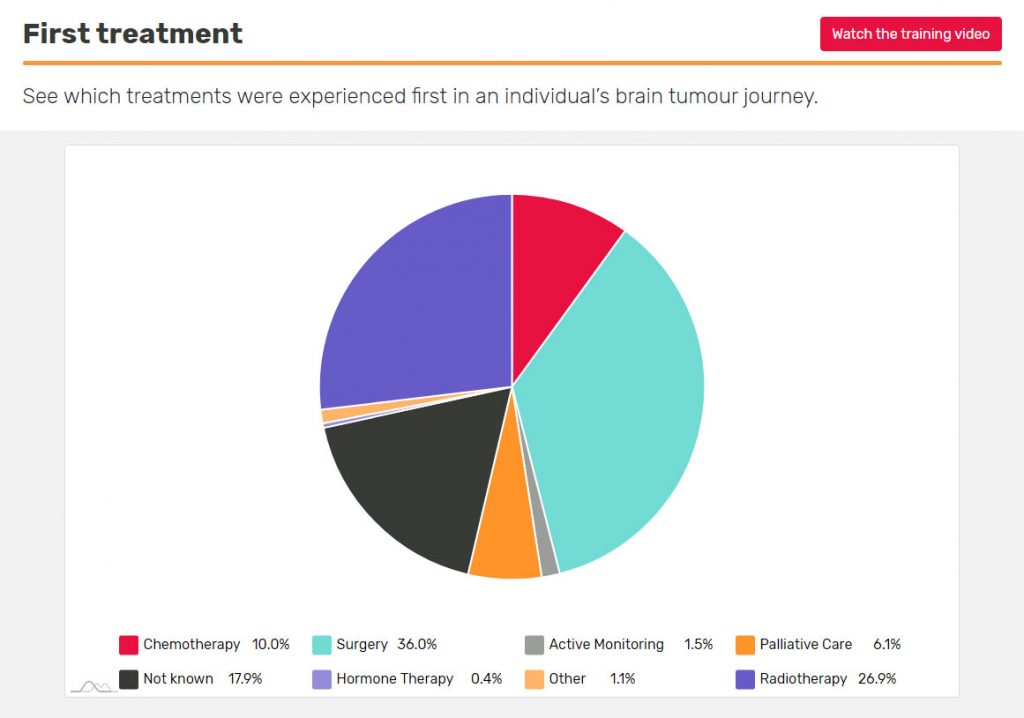
What treatment do people diagnosed with an oligodendroglioma usually have first?
If you’ve just been diagnosed with an oligodendroglioma and are about to have treatment, you may want to see what other people’s first treatment was. Use the First Treatment insight in BRIAN, which you can personalise to make it relevant to you.
Support and Information Services
Research & Clinical Trials Information
You can also join our active online community.
In this section

Get support
If you need someone to talk to or advice on where to get help, our Support and Information team is available by phone, email or live-chat.
