Meningioma
A meningioma is a type of brain tumour that begins in the meninges, the membranes that cover the brain. These tumours differ in grade and type, but are usually low grade. Relatively common, around 27% of all brain tumours diagnosed are meningiomas. They’re more common in women than men and are rare in children.
Short summary
Meningioma is a brain tumour that takes its name from the meninges – the brain membranes where this type of tumour starts.
These tumours are usually low grade and slow growing, but some can be high grade and grow quicker. That being said, there are no grade 4 meningiomas.
These tumours are more common in women than men. And, they’re often found in older people, but can affect people of any age. But, they are rare in children.
Symptoms can include headaches, vision changes, hearing loss, and more. Treatment often depends on the grade and behaviour of the tumour, but can range from active monitoring to surgery and radiotherapy.
On this page, we’ll cover:
- What is a meningioma?
- What are the meningioma symptoms?
- What causes meningioma?
- How is a meningioma treated?
- How long can I live with a meningioma?
Get support
It’s normal to feel shocked if you or someone you know has been diagnosed with a brain tumour. Our Support Team can answer questions you have or provide a listening ear if you need one.
Get your free Information Pack
Our Brain Tumour Information Pack can help you better understand your diagnosis and feel confident talking to your medical team.
Get the BRIAN app
BRIAN is our trusted online app where you can track your experience, compare it with others who’ve been there and get the knowledge you need to make informed decisions.
What is a meningioma?
A meningioma (pronounced men-in-gee-oh-ma) is a tumour that grows in the set of three membranes just inside the skull, called the meninges. The function of these membranes is to cover and protect the brain and spinal cord.
Meningiomas can be grades 1, 2 or 3, but there are no grade 4 ones. Within these grades, there are also different types, which you may hear during your diagnosis or during consultations with your healthcare team.
Meningiomas are usually:
- low grade tumours
- slow growing
- unlikely to spread.
But, some types don’t behave as expected and can grow quicker than others.
-
Grade 1 meningiomas are the most common and may not cause symptoms for many years after diagnosis. So, immediate treatment is not always needed.
Some of the different types of grade 1 meningioma are:
- meningothelial
- fibrous
- transitional
- psammomatous
- angiomatous
- microcystic
- secretory
- lymphoplasmacyte-rich
- metaplastic.
-
These are slow growing, but may be more likely to come back after treatment, possibly as a higher grade.
Some of the different types of grade 2 meningioma are:
- chordoid
- clear cell
- atypical.
-
These are very rare and faster growing, with a higher chance of recurring after treatment.
Some of the different types of grade 3 meningioma are:
- papilliary
- rhabdoid
- anaplastic.
What are the meningioma symptoms?
These tumours can often be present in the brain without causing any symptoms for many years.
Meningioma symptoms usually begin gradually, as they gently push and compress brain tissue, rather than invading it. As with other brain tumours, the symptoms will depend on which part of the brain is affected.
That being said, meningioma symptoms could include:
- Headaches
- Change in vision, like partial loss of vision or double vision
- Cognitive difficulties like memory loss
- Hearing loss or ringing in the ears
- Loss of smell
- Seizures (epilepsy)
- Feeling weak in your limbs

Five years ago I felt like my life was over, but now, despite everything, I’m really happy.
Susan

Susan Jones, diagnosed with a meningioma in 2014
“When I started suffering with headaches, fatigue and memory problems, I put my symptoms down to my age and the menopause. But when I started falling over, slurring my speech and couldn’t raise my arm, my daughter insisted I visited my GP and pushed for me to have an MRI scan.
“It was discovered that I had a meningioma on my left frontal lobe. Following surgery I lost the ability to speak, read, spell or even tell the time, and it greatly affected my memory. But I was determined to get my life back on track and after 18 months of rehabilitation, my speech and memory are much better.
“I’m now 60 and back at work. I split the rest of my time between writing books, volunteering and having fun with friends and family.
“It can be easy to think a diagnosis means your life is over, but there are still happy times to come – don’t give up! Find a goal, something to move forward for, and go for it. All any of us have is right now, and you have to keep picking yourself up and moving forwards.“
Join one of our Online Support Communities for more stories and tips about coping with a brain tumour diagnosis from people who know what you’re going through.
What causes meningioma?
As with all brain tumours, the answer is we don’t yet know.
It’s important to know there is nothing you could have done, or avoided doing, that would have caused you to develop a brain tumour.
Research is ongoing to find out the causes and help to develop treatment targeted at these.
We are starting to learn some of the risk factors. A risk factor is something that increases your chance of developing a tumour, but most do not directly cause the tumour.
This means that some people with several risk factors may never develop a tumour, while others with no known risk factors do develop a tumour.
-
Age
Theare more common in people aged over 50, and particularly in people over 65 years.
Gender
Grade 1 meningiomas are more common in women and it’s thought that this may be linked to female hormones. Grade 2 meningiomas are equally common in men and women. Grade 3 meningiomas are much more common in men than in women.
Hormones
As well as being more common in women, it‘s also been noted that occasionally meningiomas can grow faster during pregnancy. Some studies have also suggested a link between breast cancer and meningioma risk.
In addition, it’s been found that some meningiomas have specialised cells (called receptors) that interact with the female hormones, progesterone and oestrogen. This has led doctors to believe that female hormones may play a role in increasing your risk of developing this tumour type.
Research is looking at the role of hormones in the growth of meningiomas to understand the significance of this.
Radiation treatment
Exposure to radiation, particularly to the head and particularly in childhood, may increase the risk of developing a meningioma later in life. This could include accidental exposure to radiation or radiation therapy as a treatment for various medical conditions.
Obesity
Women who have a body mass index (BMI) of 30 or more have a 60% higher risk of developing a meningioma than women who have a BMI of between 18.5 and 24.9.
This is thought to be due to the fact that fatty tissue produces hormones such as oestrogen.
Genetics
A small number of brain tumours occur as a result of rare genetic conditions.
For example, the rare condition neurofibromatosis type 2 (NF2) causes (usually low grade) tumours to grow along the nerves, including those in the brain and spinal cord. As a result, it’s known to increase the risk of developing brain tumours, including meningiomas.
Did you know that we have an Online Support Group specifically for people affected by a meningioma diagnosis?
How is a meningioma treated?
Meningiomas are normally treated according to their grade. But their location, size, and the symptoms you’re having will also affect which treatment you’re offered.
People who are diagnosed with a grade 1 meningioma are often put on active monitoring treatment (also known as ‘watch and wait’), with surgery and radiotherapy offered at a later date, if needed.
Grade 2 and 3 types usually have surgery, then radiotherapy.
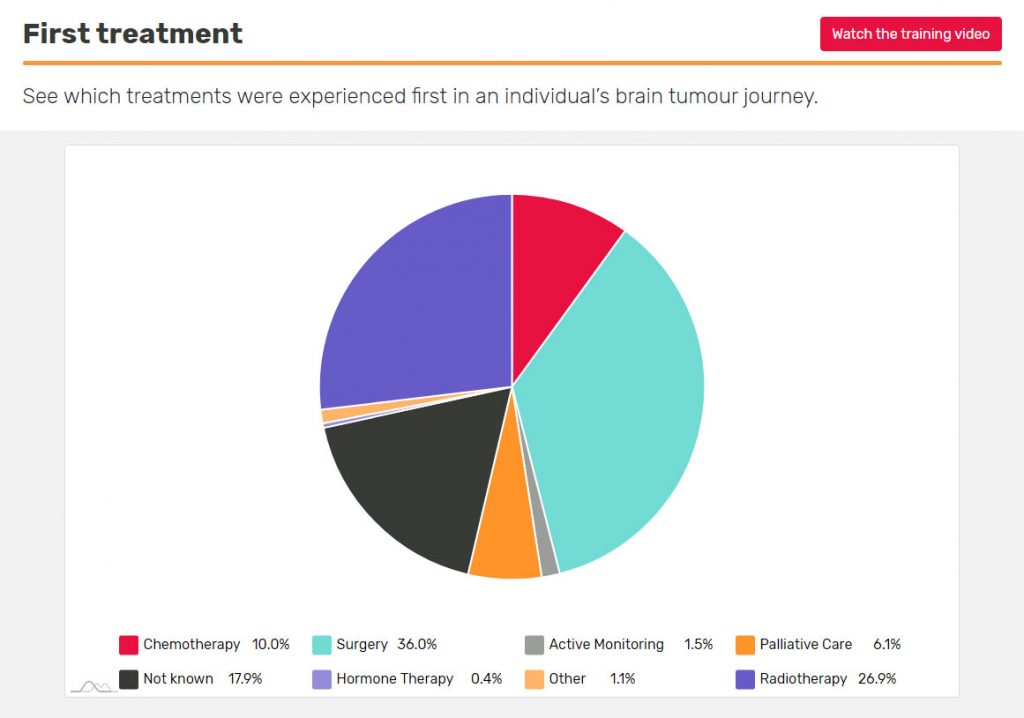
What treatment do people diagnosed with a meningioma usually have first?
If you’ve just been diagnosed with a brain tumour and are about to have treatment, you may want to see what other people’s first treatment was. Use the First Treatment insight in BRIAN, which you can personalise to make it relevant to you.
How long can I live with a meningioma?
As with all brain tumours, this is difficult to answer. Your doctor can give you an estimate, based on your tumour grade, location and current health. But they may not be able to predict other factors, like how fast it might grow or how well you could respond to treatment.
Download our factsheet
Meningioma factsheet – PDF
Find out more about meningiomas, including symptoms, treatments and risk factors in our new meningioma factsheet.
Support and Information Services
Research & Clinical Trials Information
You can also join our active online community.
In this section

Get support
If you need someone to talk to or advice on where to get help, our Support and Information team is available by phone, email or live-chat.
Recommended reading

Share your experiences and help create change
By taking part in our Improving Brain Tumour Care surveys and sharing your experiences, you can help us improve treatment and care for everyone affected by a brain tumour.
